 Diagnostics · NYC
Diagnostics · NYC
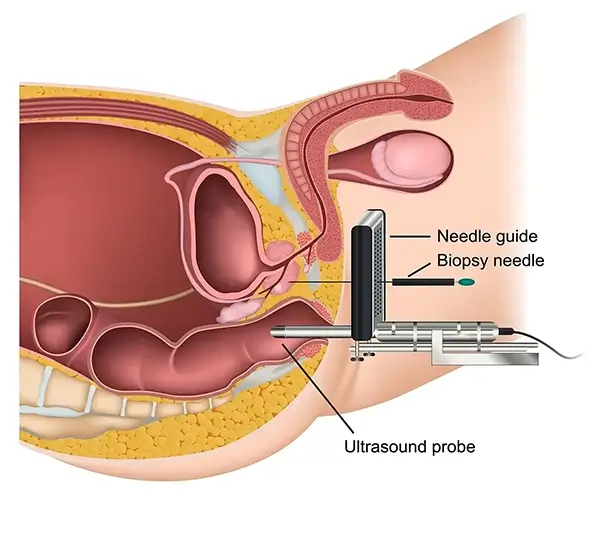
Transperineal MRI/US Fusion Prostate Biopsy
A transperineal prostate biopsy samples the prostate through the skin between the scrotum and anus — not through the rectum — under MRI/ultrasound fusion guidance. Because the needle never crosses the rectal wall, the risk of sepsis is essentially eliminated and antibiotics are not routinely required.
Dr. Tan performs 500+ transperineal biopsies per year in an office setting, with a published mean pain score of 1.8 / 10 without sedation. Local anesthesia. Walk-out the same day. Pronox (nitrous oxide) is available for anxious patients.
“Going through the rectum is like going through the sewer to get into one's home.”— Dr. Wei Phin Tan, MD, MHS, FACS
Transperineal vs. Transrectal Biopsy
| Transperineal (Dr. Tan) | Transrectal | |
|---|---|---|
| Infection Rate | Near zero | 5–7% |
| Sepsis Risk | Near zero | 1–2% |
| Antibiotics | None required | Required |
| Enema | Yes — improves visualization | Required |
| Anesthesia | Local (office) | Varies |
| Cancer Detection | Equivalent or better | Baseline |
What Makes This Different
- Office-based under local anesthesia — no operating room, no general anesthesia
- MRI fusion-guided — targeted sampling of MRI-visible lesions
- Published pain score 1.8 / 10 without sedation
- Pronox (nitrous oxide) available for anxious patients
- No antibiotics because the needle avoids the rectal wall
- 500+ procedures per year — volume with outcomes
What to Expect
- Consultation. Review PSA trend, prior imaging, and risk factors.
- MRI. A multiparametric MRI is obtained if not already available.
- Biopsy day. Enema, local anesthesia, office-based procedure. Pronox available on request.
- Pathology. Results reviewed with you in follow-up — with integrated discussion of next steps, from surveillance to focal therapy to surgery.